A Loose Tooth Is More Than a Minor Nuisance
Tooth mobility is rarely just a harmless wobble; it signals that the supporting structures—bone, ligament, and gum tissue—are deteriorating. This can stem from periodontal disease, trauma, bruxism, or systemic conditions such as diabetes. If ignored, the loose tooth may progress to infection, bone loss, abscess formation, and even systemic complications like heart disease or sepsis. A dental professional will first assess the degree of mobility, take radiographs, and identify the underlying cause. Treatment may involve deep cleaning, splinting, root‑canal therapy, or extraction, often combined with antibiotics or periodontal surgery to preserve oral health and help maintain a smile for life.
Why a Loose Tooth Signals Serious Health Issues
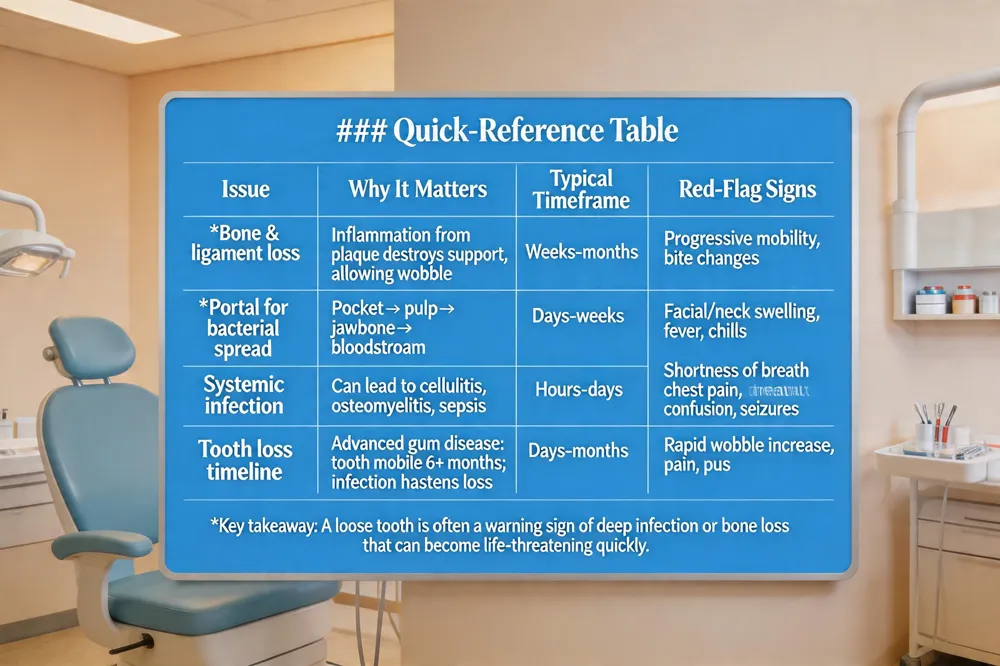
Quick‑Reference Table
| Issue | Why It Matters | Typical Timeframe | Red‑Flag Signs |
|---|---|---|---|
| Bone & ligament loss | Inflammation from plaque destroys support, allowing wobble | Weeks‑months of untreated disease | Progressive mobility, bite changes |
| Portal for bacterial spread | Pocket → pulp → jawbone → bloodstream | Days‑weeks after abscess forms | Facial/neck swelling, fever, chills |
| Systemic infection | Can lead to cellulitis, osteomyelitis, sepsis | Hours‑days once bacteria enter bloodstream | Shortness of breath, chest pain, confusion, seizures |
| Tooth loss timeline | Advanced gum disease may keep tooth mobile 6+ months; infection can hasten loss | Days‑months | Rapid increase in wobble, pain, pus |
Key takeaway: A loose tooth is often a warning sign of deep infection or bone loss that can become life‑threatening quickly.
 A loose tooth is often the first visible sign of advanced periodontal disease. When plaque and tartar are not removed, inflammation destroys the supporting bone and ligament, allowing the tooth to wobble. As the bone recedes, neighboring teeth lose their anchor, creating bite problems and increasing the risk of further loss.
A loose tooth is often the first visible sign of advanced periodontal disease. When plaque and tartar are not removed, inflammation destroys the supporting bone and ligament, allowing the tooth to wobble. As the bone recedes, neighboring teeth lose their anchor, creating bite problems and increasing the risk of further loss.
The loosened tooth also creates a portal for bacteria to travel from the gingival pocket into the pulp and surrounding tissues. If the infection breaches the tooth’s protective barriers, it can spread to the jawbone, form an abscess, and eventually enter the bloodstream. This pathway can trigger systemic conditions such as cellulitis, osteomyelitis, or sepsis—life‑threatening complications that may develop within days after an abscess forms.
How long until a tooth infection kills you? Usually weeks to months to develop an abscess; once it spreads, death can occur within days without emergency care.
Symptoms of infection spreading: Facial or neck swelling, fever, chills, fatigue, difficulty swallowing, trismus, and lymph‑node tenderness; severe signs include shortness of breath, chest pain, confusion, or seizures.
Dental emergency definition: Any condition requiring immediate attention—uncontrolled bleeding, severe throbbing pain, knocked‑out or cracked teeth, abscess with swelling/fever, or deep oral injuries.
How long does a loose tooth take to fall out in adults? From a few days to several months, depending on cause; untreated advanced gum disease can keep a tooth mobile for six‑plus months, while infection may accelerate loss.
Immediate Actions You Can Take at Home
Home‑Care Action Table
| Action | How To Do It | Purpose |
|---|---|---|
| Gentle brushing | Soft‑bristled brush, fluoride toothpaste, twice daily | Remove plaque without aggravating mobility |
| Floss carefully | Use floss or interdental brush around the loose tooth | Clean interdental spaces, reduce bacterial load |
| Salt‑water rinse | ½ tsp salt in 8 oz warm water, rinse 2×/day | De‑inflammation, mild antiseptic effect |
| Temporary floss splint | Loop clean floss around loose tooth, tie loosely to adjacent stable tooth | Limit motion, give ligament a chance to heal |
| Soft‑food diet | Yogurt, mashed potatoes, scrambled eggs, smoothies | Reduce mechanical stress on the tooth |
| Pain control | Ibuprofen 600 mg every 6‑8 h (max 3 days) | Manage inflammation and discomfort |
| Avoid chewing on affected side | Stick to opposite side for meals | Prevent further trauma |
These steps keep the area clean and stable while you arrange a dental appointment.
 When a tooth feels wobbly, start with gentle oral care. Brush twice daily with a soft‑bristled toothbrush and fluoride toothpaste, floss carefully, and rinse twice a day with warm salt‑water (½ tsp salt in 8 oz water) to reduce inflammation and bacterial load. For a quick, temporary splint, loop a clean piece of dental floss around the loose tooth and loosely secure it to an adjacent stable tooth; this limits motion while the supporting ligaments begin to heal. Adjust your diet to keep pressure off the tooth—choose soft foods such as yogurt, mashed potatoes, scrambled eggs, and avoid hard, sticky, or very acidic items.
When a tooth feels wobbly, start with gentle oral care. Brush twice daily with a soft‑bristled toothbrush and fluoride toothpaste, floss carefully, and rinse twice a day with warm salt‑water (½ tsp salt in 8 oz water) to reduce inflammation and bacterial load. For a quick, temporary splint, loop a clean piece of dental floss around the loose tooth and loosely secure it to an adjacent stable tooth; this limits motion while the supporting ligaments begin to heal. Adjust your diet to keep pressure off the tooth—choose soft foods such as yogurt, mashed potatoes, scrambled eggs, and avoid hard, sticky, or very acidic items.
How to tighten a loose tooth fast – Schedule a dental appointment promptly; in the meantime keep the area clean, use salt‑water rinses, avoid chewing on the affected side, and eat soft foods. A dentist can apply a professional splint, deep‑clean gum pockets, or prescribe antibiotics to promote rapid re‑attachment.
How to tighten a loose tooth at home – Maintain meticulous hygiene with gentle brushing, flossing, and salt‑water rinses; use a temporary floss splint and soft‑food diet. If mobility persists beyond a few days, seek professional care.
Tooth is loose but still attached (adults) – Stop chewing on that side, keep the area clean, use salt‑water rinses, and book a dental evaluation to identify cause and receive splinting or periodontal therapy.
My front tooth is loose—what can I do? – Avoid touching or wiggling the tooth, eat soft foods on the opposite side, rinse with salt water, and contact a dentist immediately for splinting or periodontal treatment.
When to Seek Professional Care
Red‑Flag Symptoms & Recommended Action
| Symptom | Why It’s Urgent | Immediate Step |
|---|---|---|
| Sudden, pronounced mobility + pain | Possible acute periodontal breakdown | Call dentist ASAP |
| Facial or neck swelling, fever, chills | Infection may be spreading systemically | Seek emergency dental/medical care |
| Pus, foul taste, throbbing pain | Abscess formation | Arrange urgent appointment; may need antibiotics & drainage |
| Difficulty swallowing, trismus, shortness of breath | Airway compromise risk | Go to emergency department immediately |
| Uncontrolled bleeding after trauma | Vascular injury | Emergency care needed |
Do NOT attempt DIY extraction; it can cause bone damage, root fracture, and severe infection.
 Red‑flag symptoms – Sudden, pronounced mobility accompanied by pain, swelling, bleeding, fever, a foul taste, or pus are warning signs of infection or severe periodontal disease. If the tooth feels extremely loose, especially after trauma, or if you experience facial swelling, difficulty swallowing, or breathing, treat it as an emergency and call a dentist immediately.
Red‑flag symptoms – Sudden, pronounced mobility accompanied by pain, swelling, bleeding, fever, a foul taste, or pus are warning signs of infection or severe periodontal disease. If the tooth feels extremely loose, especially after trauma, or if you experience facial swelling, difficulty swallowing, or breathing, treat it as an emergency and call a dentist immediately.
Risks of DIY extraction – Pulling a loose adult tooth at home can damage surrounding bone, fracture the root, or spread infection to the jaw and bloodstream. Uncontrolled bleeding and dry‑socket formation are common complications. Instead, keep the area clean with gentle brushing and warm salt‑water rinses while you arrange a professional evaluation.
Diagnostic steps a dentist takes – The clinician will perform a visual exam, probe tooth mobility, and likely obtain periapical X‑rays or a CBCT scan to assess bone loss, root fractures, or abscess formation. Periodontal probing, gum assessment, and sometimes pulp testing help pinpoint the cause—periodontitis, trauma, bruxism, or systemic factors—guiding treatment such as scaling, splinting, root canal therapy, or extraction.
My tooth is loose, can I pull it out? – No. Do not extract it yourself; seek dental care. Until then, eat soft foods, avoid wiggling, and rinse with salt water.
How do I know if there's an infection? – Look for throbbing pain, swelling, fever, pus, or a foul taste. Any of these warrant prompt dental attention.
When should you worry about a loose tooth? – Any noticeable looseness with pain, swelling, bleeding, or recent injury requires a prompt dental appointment.
How to remove a loose tooth in adults – Only a dentist should extract it, using anesthesia and sterile instruments. Post‑extraction care includes soft foods, salt‑water rinses, and any prescribed medication.
Understanding Treatment Options
Treatment Options Overview
| Option | Indication | Typical Procedure |
|---|---|---|
| Splinting (flexible or rigid) | Trauma‑related mobility, early periodontitis | Wire or fiber‑reinforced splint attached to adjacent teeth |
| Root canal therapy | Pulp infection, necrosis, abscess | Remove pulp, clean canal, obturate, place crown |
| Systemic antibiotics | Acute infection, abscess risk | Amoxicillin or clindamycin (prescribed) |
| Scaling & root planing | Moderate‑to‑severe periodontitis | Deep cleaning of plaque/tartar from tooth surfaces and roots |
| Flap surgery | Advanced bone loss, deep pockets | Surgical access to clean roots, reshape gum tissue |
| Bone grafts | Insufficient alveolar bone for support | Place graft material to encourage new bone growth |
| Extraction | Non‑restorable tooth, severe infection | Anesthesia, sterile forceps, post‑extraction care |
The dentist will choose based on X‑ray/CBCT findings, mobility grade, and infection status.
 When a tooth becomes loose, the first step is to identify the cause—periodontal disease, trauma, or infection—and then choose the appropriate stabilizing and therapeutic approach.
When a tooth becomes loose, the first step is to identify the cause—periodontal disease, trauma, or infection—and then choose the appropriate stabilizing and therapeutic approach.
Splinting and stabilization techniques: For trauma‑related mobility, dentists often splinting the tooth to neighboring healthy teeth using flexible or rigid wires, allowing the periodontal ligament to heal while preventing further displacement.
Root canal, antibiotics, and surgical options: If infection is present, a root canal removes necrotic pulp and eliminates bacteria, followed by a crown to restore strength. Systemic antibiotics (e.g., amoxicillin) may be prescribed to control spread, especially when an abscess forms. In advanced gum disease, deep cleanings (scaling and root planing), flap surgery, or bone grafts are used to rebuild support.
Guidelines for managing pain and infection at home: The "3‑3‑3 rule" recommends three 600‑mg doses of ibuprofen or naproxen three times daily for three days while arranging a dental appointment. Warm salt‑water rinses, cold compresses, and clove‑oil dab can ease discomfort but do not replace professional care.
Frequently asked questions:
- What is the 3‑3‑3 rule for tooth infection? It is a short‑term analgesic protocol to reduce pain and swelling while you seek definitive treatment.
- Tooth infection antibiotics online – Tele‑health platforms can prescribe antibiotics after a clinician evaluates your symptoms, but an in‑person exam is still required for drainage or root canal therapy.
- How to get rid of a tooth abscess without going to the dentist – Home rinses and pain relievers may relieve symptoms temporarily; definitive treatment (drainage, root canal, or extraction) must be performed by a dentist.
- Dentist in Paterson, NJ – Dr. David Mayer, DMD, offers emergency and routine care at 1010 Main St, Suite 8, with bilingual staff and modern technology.
- Dentist Paterson, NJ Main St – Same practice provides comprehensive services, including same‑day emergency appointments, to address loose teeth promptly.
Local Resources and Frequently Asked Logistics
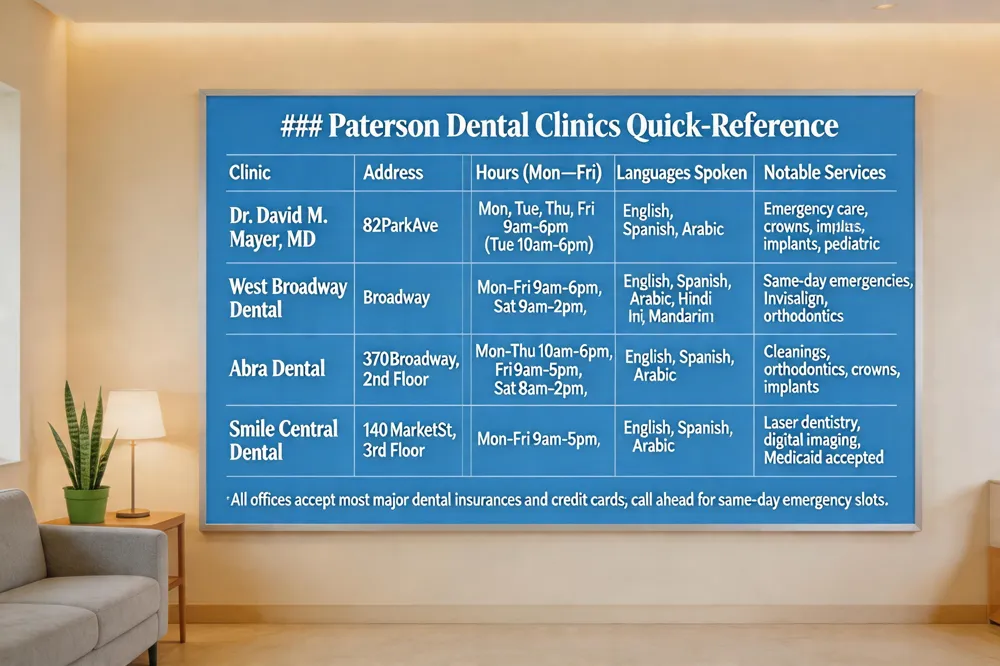
Paterson Dental Clinics Quick‑Reference
| Clinic | Address | Hours (Mon‑Fri) | Languages Spoken | Notable Services |
|---|---|---|---|---|
| Dr. David M. Mayer, MD | 82 Park Ave | Mon, Tue, Thu, Fri 9 am‑6 pm (Tue 10 am‑6 pm) | English, Spanish, Arabic | Emergency care, crowns, implants, pediatric |
| West Broadway Dental | Broadway (exact number not given) | Mon‑Fri 9 am‑6 pm, Sat 9 am‑2 pm | English, Spanish, Arabic, Hindi, Mandarin | Same‑day emergencies, Invisalign, orthodontics |
| Abra Dental | 370 Broadway, 2nd Floor | Mon‑Thu 10 am‑6 pm, Fri 9 am‑5 pm, Sat 8 am‑2 pm | English, Spanish, Arabic | Cleanings, orthodontics, crowns, implants |
| Smile Central Dental | 140 Market St, 3rd Floor | Mon‑Fri 9 am‑5 pm (typical) | English, Spanish, Arabic | Laser dentistry, digital imaging, Medicaid accepted |
All offices accept most major dental insurances and credit cards; call ahead for same‑day emergency slots.
 Paterson residents have several convenient dental options.
Paterson residents have several convenient dental options.
82 Park Ave, Paterson, NJ – Dr. David M. Mayer, MD, operates a full‑service office at 82 Park Ave, offering routine exams, cleanings, emergency care, crowns, implants, dentures and pediatric services. Hours: Mon, Tue, Thu, Fri 9 am‑6 pm (Tue starts at 10 am); closed Wed, Sat, Sun. The multilingual team speaks English, Spanish and Arabic and accepts most dental insurances and credit cards.
Broadway, Paterson, NJ – West Broadway Dental on Broadway provides adult and family care, including cleanings, crowns, implants, dentures, orthodontics, Invisalign and same‑day emergencies. The 25‑room clinic runs with staff fluent in English, Spanish, Arabic, Hindi and Mandarin, and accepts United Healthcare, Amerigroup, Medicaid, Horizon, Wellcare and other major plans.
Abra Dental, Paterson, NJ – Located at 370 Broadway, 2nd Floor, Abra Dental offers cleanings, exams, pediatric,, orthodontics, crowns and implants. Hours: Mon‑Thu 10 am‑6 pm, Fri 9 am‑5 pm, Sat 8 am‑2 pm; multilingual (English, Spanish, Arabic) and accepts most insurances.
Smile Central Dental, Paterson – At 140 Market St, 3rd Floor, this practice provides general, pediatric, orthodontic and restorative services with laser and digital tech. English, Spanish and Arabic are spoken; Medicaid‑accepting offices include West Broadway Dental, New Smile Dentistry, Hello Dental – Haledon, and Union Dental – Donald Pasquariello DMD.
Don’t Let a Loose Tooth Slip Away
A loose tooth is rarely harmless; it often signals advanced gum disease, trauma, or infection that can quickly spread to bone, gums, and even the bloodstream. If untreated, the tooth may shift, causing bite problems, damage to neighboring teeth, chronic pain, and the need for costly procedures such as extractions, bone grafts, or implants. Systemic complications—including heart disease, diabetes flare‑ups, and serious infections like cellulitis—are also linked to persistent oral inflammation. Because the underlying cause can be identified and treated early, schedule a dental evaluation within 24‑48 hours. Prompt professional care can stabilize the tooth, prevent infection, and preserve your oral health.
